
4 min|Dr. Jam Caleda
History of Platelet-Rich-Plasma (PRP) Therapy
Regenerative Injection TherapyPlatelet rich plasma (PRP) is a treatment that has gained popularity in recent years for its potential to accelerate the healing process of certain injuries and promote tissue regeneration.
PRP is an injectable product derived from a patient’s own blood that contains a high concentration of platelets, growth factors, and some circulating stem cells, which are known to play a crucial role in wound healing and tissue repair.
Although seemingly novel in a conventional medical model, PRP dates back several decades, and its development is closely tied to the advancements in medical technology and understanding of the body’s healing processes.
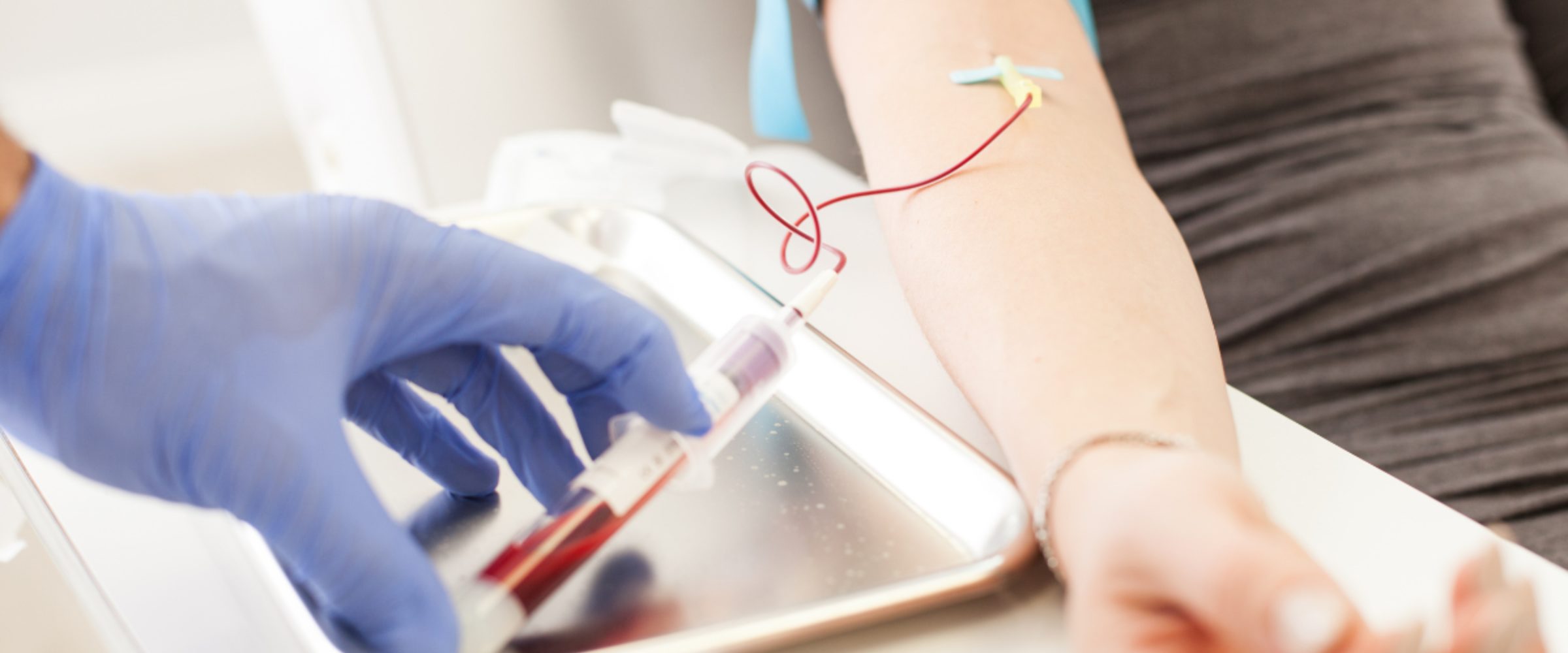
The first recorded use of PRP can be traced back to the 1970s when hematologists began to study the role of platelets in blood clotting and wound healing.
Platelets are blood cells that play a vital role in the clotting process, helping to stop bleeding and prevent further damage to injured tissues. Researchers discovered that platelets secrete growth factors, which are proteins that can stimulate the growth of new cells and tissues, as well as other bioactive substances, called chemokines, that can promote tissue repair (1).
In the 1980s, PRP began to be used as a treatment for dental and maxillofacial surgery, with researchers finding that it could help speed up the healing process and reduce the risk of infection. Until now, the procedure of using PRP in dental procedures is relatively common. The first documented use of PRP in orthopaedics and sports medicine was in the early 1990s, when it was used to treat muscle and joint injuries in professional athletes.
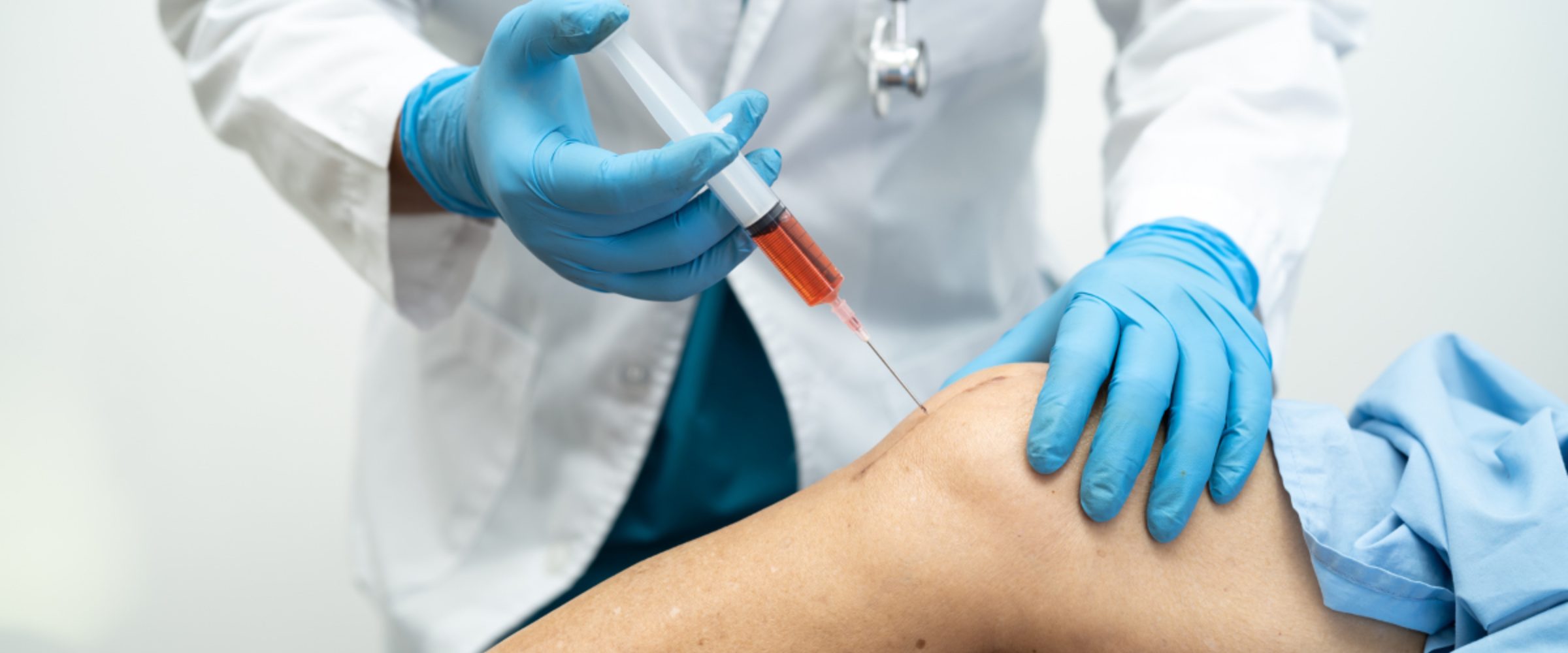
The use of the procedure in sports medicine quickly gained popularity as a non-invasive procedure to aide in healing. Many athletes and sports teams used PRP and similar injection therapies in hopes that it would speed a return to play after an injury, and in some cases their overall performance on the field.
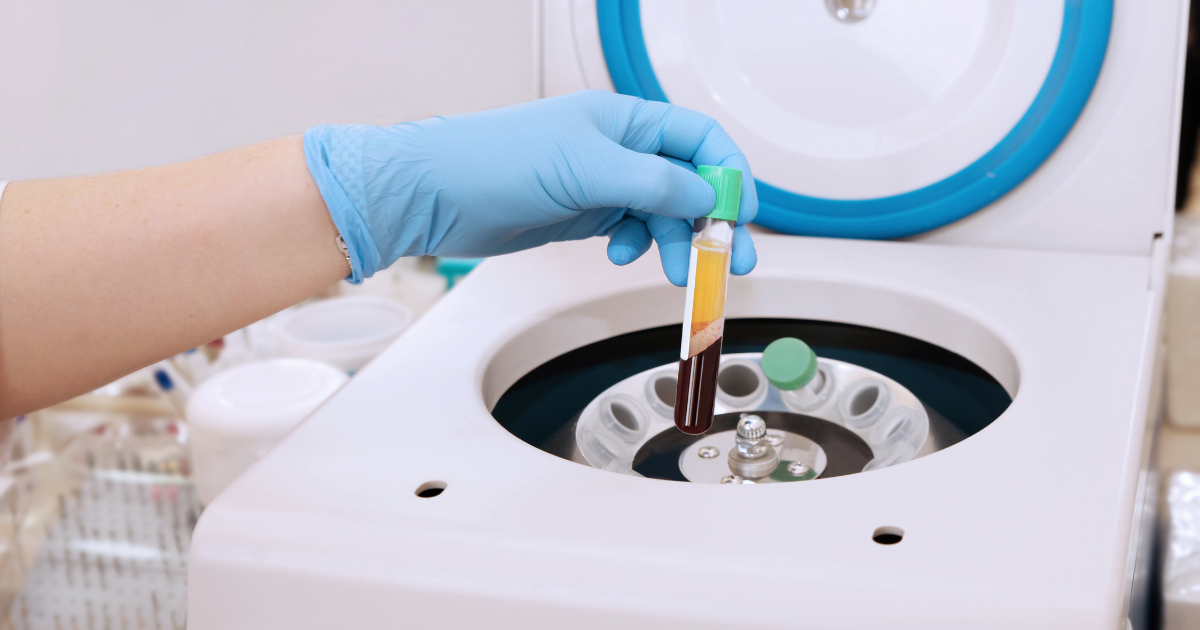
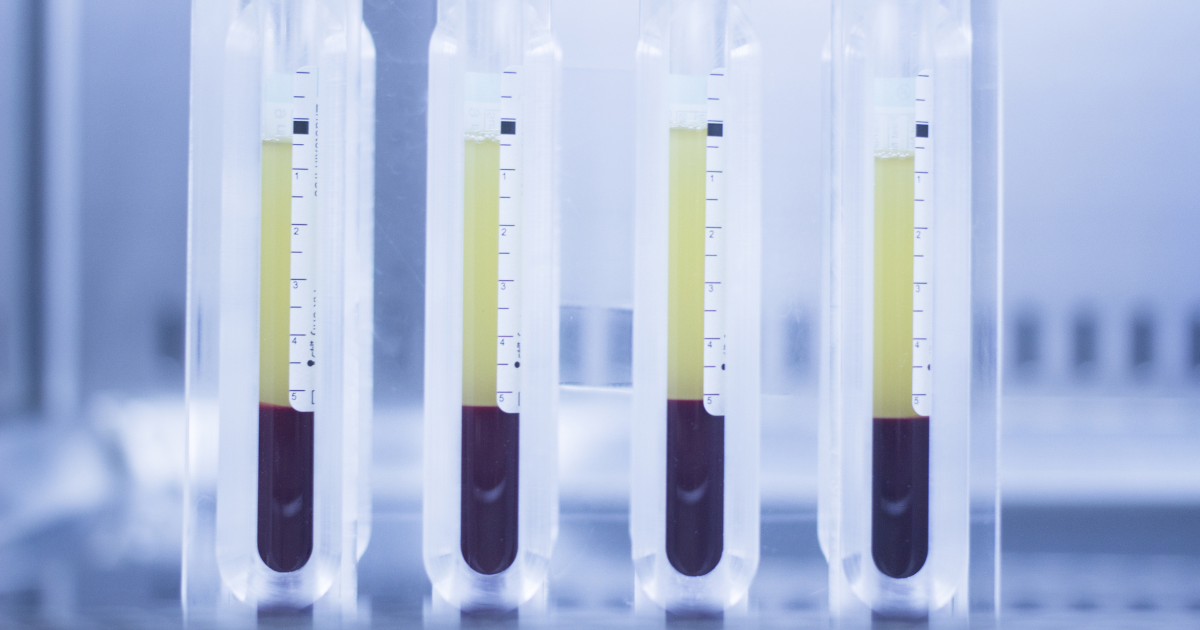
Over the years, PRP has been used to treat a wide range of injuries and conditions, including arthritis, tendonitis, ligament injuries, and muscle strains. The treatment involves drawing a small amount of blood (50-200mls) from the patient and then processing it in a centrifuge to separate the platelets from other hematological components that are not needed for regeneration. This resulting concentration of platelets and growth factors are injected directly into areas of injury, usually non-contractile tissues, to stimulate regeneration.
Benefits of PRP
One of the key benefits of PRP is that it is a minimally invasive procedure that can be performed in an outpatient setting. Recovery length is also a favorable factor, with recovery taking several days compared to a surgical recovery of several months. Physiotherapy, massage, and other physical rehabilitation can be performed concomitantly while recovering and further speed up healing from the procedure. Relative risk is also low, as the injectant is derived from the patient’s blood. Much of the risk is dependent on practitioner skill and experience, rather than the intrinsic nature of the procedure.
Within the last decade, PRP is the subject of controversy in conventional medical fields, with some experts questioning its effectiveness and safety. Critics argue that there is not enough robust scientific evidence to support the use of PRP for many conditions it is proposed for. There is also concern for a strong bias of practitioners who perform the procedure, toting case studies that yield miraculous outcomes. Others have raised concerns about the potential risks of PRP, such as infection and nerve damage, although these events and risks are generally considered to be rare and low.
Despite these criticisms, PRP continues to be used as a treatment for a variety of musculoskeletal conditions, and research into its effectiveness and safety is on-going. In more recent years, researchers have begun to explore the use of PRP in combination with other biological treatments, such as stem cell therapy, to further potentiate regenerative capacity of the tissues treated.
The development of PRP has been closely tied to advances in medical technology and understanding of the body’s healing processes. As our knowledge of the role of platelets and growth factors in tissue repair continue to grow, it is likely that PRP will become an even more widely used and effective treatment option in the future. While there is still much to learn about PRP, its history is a testament to the power of medical research and innovation in improving our ability to treat and heal injuries.
References:
1. Alves R, Grimalt R. A review of platelet-rich plasma: history, biology, mechanism of action, and classification. Skin appendage disorders. 2018;4(1):18-24.
Related Articles
4 min|Dr. Alex Chan
EBOO for Chronic Inflammation: A Natural Approach for Systemic Relief
Regenerative Medicine, EBOO Therapy
4 min|Dr. Alex Chan
EBOO Therapy for Autoimmune Conditions: Exploring the Potential Benefits
Autoimmune Disease, Regenerative Medicine, EBOO Therapy



