Welcome to Integrative Naturopathic Medical Centre in Vancouver
Integrating traditional and conventional medicines to treat the root of illness and disease. Proudly serving Vancouver, BC for over 35 years.
Vancouver's award-winning Naturopathic Clinic with a dedicated team of Naturopathic Doctors and staff, providing patient-centred integrated health services.
1 of 3
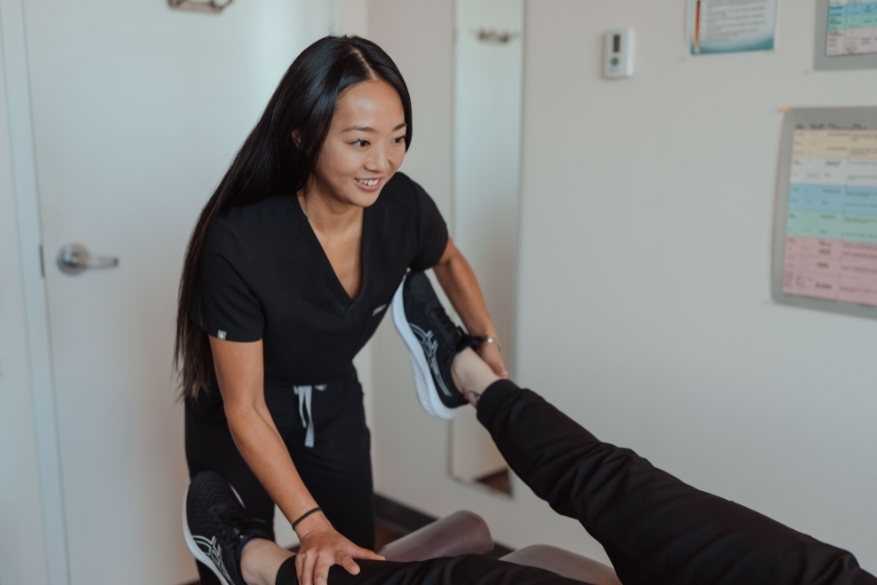
Over 35 years of expertise
At Integrative, we offer comprehensive and individualized health plans founded with over 35 years of expertise.
2 of 3
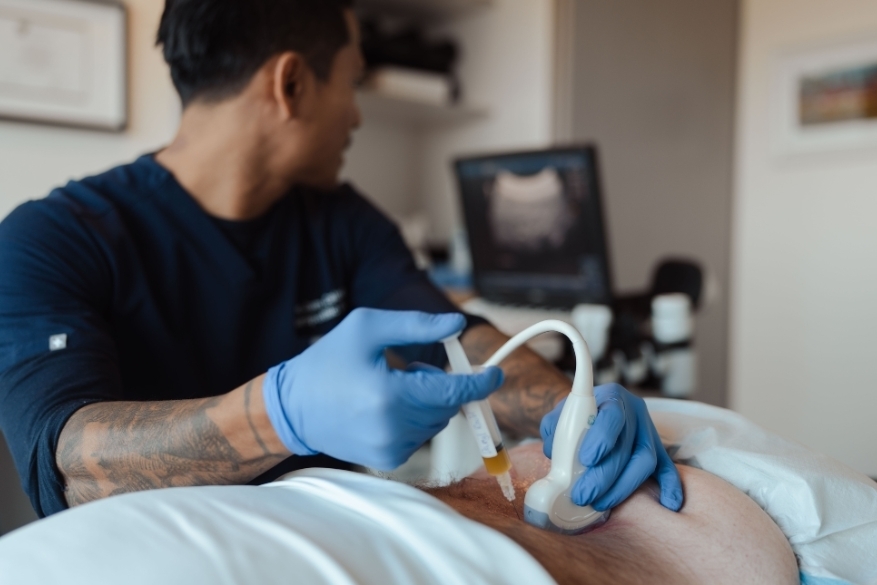
A focus on treating the root cause
Addressing the origins of your health concerns, we focus on the root cause rather than just treating the symptoms.
3 of 3
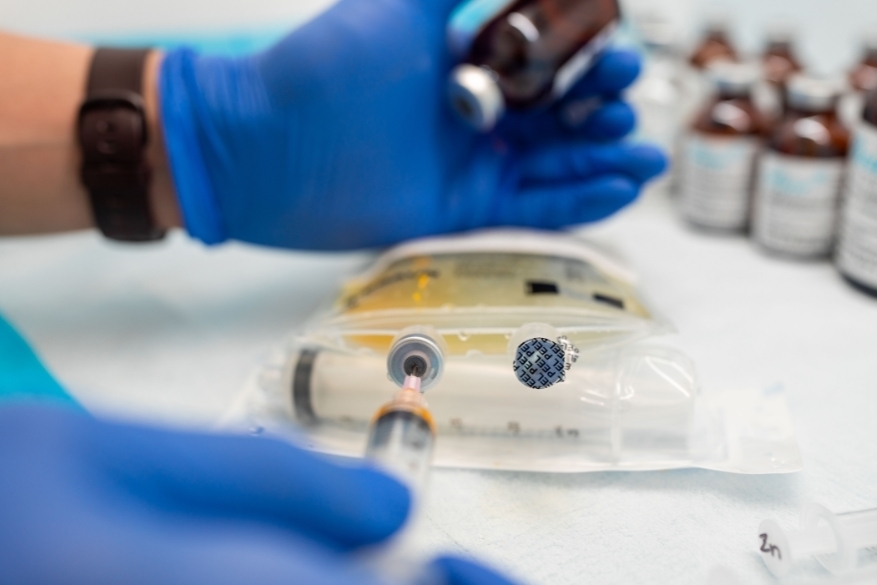
An integrative medical facility
The Integrative facility is home to the Integrative Laboratory and Integrative Natural Dispensary which are all under one roof.
Individualized health goals from experienced Naturopaths that help guide your treatment plan
Your health goals are important to us. No matter your goal, our team integrates conventional and traditional healing methods to develop your unique treatment plan.
Naturopathic treatments that combine traditional and conventional medicines
Our toolbox is vast, providing multiple treatment options that your practitioner can combine to create your treatment plan.
Latest articles
View all articles 
4 min|Dr. Taylor Green
Navigating IBS: Uncovering the Root Cause When You're Feeling Stuck
Irritable Bowel Syndrome (IBS) is a multifaceted condition diagnosed on a constellation of symptoms such as excessive chronic bloating, gas, abdominal cramping & pain, nausea, and altered bowel habits. It is considered a diagnosis of exclusion, meaning a...Read 

4 min|Dr. Jordan Dutton
A New Frontier in Bladder Care: Ozone Bladder Insufflation
Wellness, Education
4 min|Rhiannon Lockhart
Taking A Holistic Approach To Irritable Bowel Syndrome (IBS)
Health, Gut Health